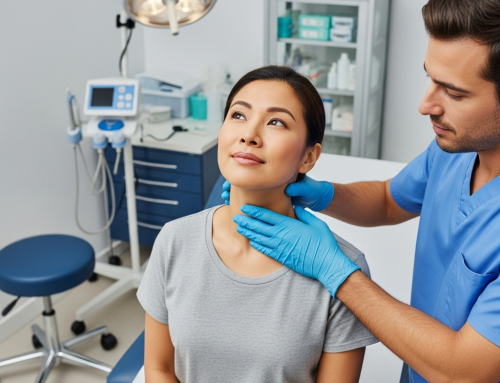
What Happens to Your Medications After an Auto Accident Injury Claim?
You’re sitting in the ER waiting room at 2 AM, ice pack pressed against your swollen knee, insurance cards scattered across your lap like confetti. The other driver’s insurance adjuster has already called twice – somehow they got your number before you even got X-rays – and you’re trying to remember if you took your blood pressure medication this morning. Or was that yesterday morning? Time gets fuzzy when you’re running on adrenaline and whatever they gave you for the pain.
Here’s the thing nobody tells you about car accidents: the crash is just the beginning. Sure, everyone talks about getting your car fixed and dealing with insurance claims, but what about the bottles of pills now lining your bathroom counter? The medications that weren’t part of your life 48 hours ago but suddenly feel as essential as morning coffee.
Maybe you’re dealing with prescription pain relievers that cost more than your grocery budget. Or anti-inflammatory drugs that your doctor prescribed to get you through the healing process. Perhaps it’s physical therapy sessions, muscle relaxants, or even mental health medications if the accident triggered anxiety or PTSD. (And honestly? That’s more common than you might think – your brain doesn’t just bounce back from trauma like nothing happened.)
The bills start arriving before your bruises fade. Your regular insurance might cover some medications, but what about the ones specifically related to your accident injuries? And here’s where it gets tricky – there’s this weird gray area where your health insurance, the other driver’s insurance, and your own auto insurance start playing a game of “not it” with your medical expenses.
I’ve seen people ration their prescribed pain medication because they couldn’t afford the co-pays. Others who stopped physical therapy halfway through because they hit their insurance limits. Some folks don’t even realize they could potentially get their accident-related medications covered through the injury claim process.
It’s like being handed a puzzle with pieces from three different boxes, and nobody bothered to show you the picture on the front.
Your medication costs after an accident aren’t just line items on a medical bill – they’re a crucial part of your recovery that deserves the same attention as getting your bumper fixed. Actually, more attention, because unlike your car’s bumper, you can’t just trade in your body for a newer model when the repairs get too expensive.
The frustrating part? Most people stumble through this process blind. They’re dealing with pain, trying to get back to work, managing insurance calls, and somewhere in that chaos, the medication piece gets overlooked until the bills pile up. Or worse – until they realize months later that they could have been documenting and claiming these costs all along.
But here’s what I want you to know: you don’t have to navigate this maze alone, and you definitely don’t have to choose between proper treatment and financial stability. The system is complicated, sure, but it’s not incomprehensible once someone explains how the pieces actually fit together.
We’re going to walk through exactly how medication costs work in accident claims – from the moment you pick up that first prescription to the final settlement check. You’ll learn which medications typically get covered, how to document everything properly (because trust me, documentation is everything), and what to do when insurance companies start playing their favorite game of “prove it.”
More importantly, we’ll talk about timing. When to pay out of pocket versus when to wait. How to coordinate between different insurance providers without losing your mind. What happens if you need long-term medications for chronic pain or ongoing issues that developed after the accident.
And yes, we’ll cover the stuff nobody likes to think about – like what happens if your case takes years to settle but you need those medications now. Or how pre-existing conditions complicate things. Real talk about real situations, because generic advice doesn’t help when you’re holding a $200 prescription receipt and wondering if you’ll ever see that money again.
Your recovery shouldn’t be held hostage by paperwork and insurance policies. Let’s figure this out together.
The Insurance Maze – Who’s Actually Paying?
Here’s where things get… well, honestly? Pretty confusing.
When you’re hurt in an accident, you’ve got multiple insurance systems that could potentially cover your medications – and they don’t always play nicely together. Think of it like having three different credit cards, each with different rules about what they’ll pay for, and sometimes they argue about who should pick up the check.
Your health insurance might cover your prescriptions initially – that’s what you’d expect, right? But here’s the twist: if your injuries are from an accident, your auto insurance’s Personal Injury Protection (PIP) or Medical Payments coverage might actually be the primary payer. And if the other driver was at fault… their liability insurance enters the chat.
It’s like a complicated dance where everyone’s stepping on each other’s toes, and you’re stuck in the middle wondering why your pharmacy is suddenly asking questions they’ve never asked before.
The Documentation Paper Trail (Yes, It’s as Tedious as It Sounds)
Every prescription bottle becomes a potential piece of evidence. I know – that sounds dramatic for your everyday blood pressure medication, but stay with me here.
Insurance companies and lawyers need to connect the dots between your accident and your medical needs. That means proving your medications are related to your injuries, not just… life. If you were taking antidepressants before the accident and your doctor increases the dose afterward due to accident-related anxiety, that adjustment could be part of your claim. But the original prescription? That’s trickier territory.
The documentation requirements can feel overwhelming – and honestly, they are. You’re dealing with
– Medical records showing when prescriptions started or changed – Pharmacy records with dates and dosages – Doctor’s notes explaining why each medication is necessary – Sometimes even receipts (because apparently keeping track of every $10 copay becomes important)
Pre-existing Conditions – The Insurance Company’s Favorite Topic
This is where things get particularly frustrating, and I want to be straight with you about it.
Insurance companies have a talent for finding pre-existing conditions. It’s like they have a sixth sense for it. Were you taking medication for chronic pain before the accident? They’ll argue that your current pain medication needs aren’t really related to the crash – they’re just a continuation of what you were already dealing with.
But here’s what’s important to understand: having a pre-existing condition doesn’t automatically disqualify you from coverage. If the accident made your condition worse – what lawyers call an “aggravation” – you may still have a valid claim for the increased medication needs.
Think of it like this… if you had a creaky knee that you managed with occasional ibuprofen, and then the accident turned that into needing prescription pain relievers and physical therapy, that difference matters. The trick is proving it, which brings us back to that lovely documentation maze.
Timing Is Everything (Unfortunately)
There’s this invisible clock ticking from the moment of your accident, and most people don’t realize it exists until it’s almost too late.
Some insurance policies have strict timeframes for reporting medication costs. Miss that window, and you might find yourself paying out of pocket for prescriptions that should have been covered. It’s not fair – you’re dealing with injuries and trying to get your life back together – but insurance companies operate on schedules, not sympathy.
Actually, that reminds me of something else that catches people off guard: the gap between when you need medications and when insurance actually pays. You might need to pay upfront and get reimbursed later… sometimes much later. That can mean fronting hundreds of dollars for medications while you wait for the insurance wheels to turn.
The Coordination of Benefits Headache
When multiple insurance policies are involved, there’s something called “coordination of benefits” – which is just a fancy way of saying “we need to figure out who pays what, and it’s going to take forever.”
Your health insurance and auto insurance might spend weeks or months playing hot potato with your claims. Meanwhile, you’re at the pharmacy counter, and they’re asking which insurance to bill, and honestly? You might not know the answer.
It’s like being asked to referee a game where you don’t know all the rules, and the stakes are whether you can afford your medication this month. Not exactly the position anyone wants to be in while recovering from an accident.
Document Everything From Day One (Yes, Even That Receipt from CVS)
Here’s what nobody tells you – that crumpled receipt from your pharmacy run at 2 AM? Keep it. I know, I know… who keeps receipts anymore? But after an accident, every single medication purchase becomes potential evidence for your claim.
Start a dedicated folder (physical or digital, whatever works for you) and toss in everything medication-related. Prescription receipts, over-the-counter purchases, even that bottle of ibuprofen you grabbed at the gas station because your back was killing you. Insurance adjusters love to play the “prove it” game, and you want to be ready.
Pro tip: Take photos of all your medications with your phone – bottles, labels, everything. If you lose a receipt or a bottle gets damaged, you’ve got backup proof sitting right in your camera roll.
Master the Art of Medical Record Requests
Your doctor’s office isn’t going to automatically send your complete medication history to your attorney – you’ll need to be proactive here. And honestly? Most people mess this part up because they don’t know what to ask for.
Don’t just request “medical records.” Be specific. Ask for your complete pharmaceutical history, medication lists from each visit, any drug interaction notes, and dosage changes. If you were prescribed something new after the accident, you want documentation showing exactly when and why.
Here’s a little insider secret… request records from your pharmacy too. They keep detailed logs that sometimes include information your doctor’s office doesn’t have. CVS, Walgreens, whoever you use – they’re required to provide you with your medication history upon request.
Timing Is Everything (And Insurance Companies Know This)
Insurance adjusters will try to argue that your medications aren’t accident-related if there’s any gap in treatment or documentation. They’re looking for reasons to minimize your claim, and medication timing is low-hanging fruit for them.
If your doctor prescribes something new three weeks after the accident, make sure the medical notes clearly connect it to your injuries. Sometimes doctors assume the connection is obvious (spoiler alert: insurance companies will pretend it’s not).
Keep a simple medication diary – when you take what, how it affects you, any side effects. Nothing fancy, just notes in your phone. “Started muscle relaxer today, helped with spasms but made me drowsy.” This creates a timeline that’s hard to dispute later.
Navigate the Pre-Existing Medication Minefield
This is where things get tricky… If you were already taking medications before the accident, insurance companies will try to exclude them from your claim. But here’s what they don’t want you to know – dosage increases or additional medications prescribed because of your injuries are absolutely claimable.
Let’s say you were taking a low dose of anti-inflammatory medication for arthritis, but after the accident your doctor doubled the dose and added a muscle relaxer. The original medication? Probably not covered. The increased dose and new prescription? Totally fair game.
Document any changes meticulously. Before the accident you took 200mg of ibuprofen twice daily – after the accident you’re taking 400mg three times daily plus a prescription pain reliever. That difference matters, and it’s worth real money in your claim.
Work Smart with Your Attorney (They’re Not Mind Readers)
Your lawyer handles dozens of cases, and they can’t possibly track every detail of your medication regimen. Make their job easier (and your outcome better) by organizing everything upfront.
Create a simple spreadsheet – medication name, prescribing doctor, dates prescribed, reason (connected to accident), cost. Update it monthly and send it to your attorney. They’ll love you for it, and it keeps your case moving forward instead of getting bogged down in documentation requests later.
Also… don’t wait until settlement negotiations to mention that expensive specialty medication your pain management doctor prescribed. These things need to be documented and calculated into your claim value early in the process.
Think Beyond the Obvious Costs
Most people only think about the prescription costs themselves, but there’s so much more that’s recoverable. Co-pays for doctor visits to get prescriptions, parking fees at medical appointments, even mileage to and from the pharmacy if you’re making special trips because of your injuries.
That pill organizer you bought because you’re suddenly managing five different medications? Claimable. The heating pad your physical therapist recommended to help with medication side effects? Potentially claimable.
Keep receipts for anything health-related that you purchased because of your accident injuries. The worst thing that happens is the insurance company says no – but you’d be surprised what they’ll actually pay for when it’s properly documented and requested.
When Your Medication Schedule Goes Off the Rails
Let’s be honest – after an accident, keeping track of your medications can feel like trying to juggle while riding a unicycle. You’re dealing with pain, insurance calls, doctor appointments… and suddenly you can’t remember if you took your morning pills or just thought about taking them.
This isn’t just about being forgetful (though that happens too). Your entire routine gets turned upside down. Maybe you’re sleeping at odd hours because of pain, or you’re stuck in a hospital bed where nurses control the medication schedule. That careful system you had – pill organizer by the coffee maker, alarms on your phone – it’s all out the window.
The solution? Start simple. Get a basic pill organizer and set just one phone alarm. Don’t try to recreate your entire pre-accident system immediately. You’re already overwhelmed. Build back slowly, one habit at a time.
The Insurance Documentation Nightmare
Here’s what nobody tells you: insurance companies want documentation for everything. And I mean *everything*. They’ll want to know about medications you were taking before the accident, medications prescribed after, dosage changes, side effects… it’s like they want a dissertation on your pharmaceutical history.
The real kicker? They often request this information when you’re least equipped to provide it. You might be on pain medication that makes you fuzzy, or dealing with injuries that make it hard to focus. Yet they need detailed records – and they need them yesterday.
Here’s your lifeline: Create a medication master list right now, before you need it. Include medication names, dosages, prescribing doctors, and pharmacy information. Keep copies in multiple places – your phone, a folder in your car, with a trusted family member. When insurance asks for documentation, you won’t be scrambling through medicine cabinets at 2 AM trying to read tiny prescription labels.
Also – and this is crucial – photograph every prescription bottle before you throw it away. Those little orange bottles contain information you might need months later for your claim.
The Pharmacy Shuffle Struggle
You know what’s maddening? When your regular pharmacy suddenly becomes “out of network” after your accident, or your insurance changes mid-treatment. Suddenly you’re standing at an unfamiliar counter, trying to explain your complex medication regimen to a pharmacist who’s never seen you before.
This happens more than you’d think. Insurance changes, you move temporarily to recover, or your doctor refers you to a specialty pharmacy for certain medications. Each transition is a potential disaster waiting to happen.
The fix isn’t glamorous, but it works: Keep a current medication list on your phone with generic names, not just brand names. Pharmacies can work with “metformin” but might get confused by “Glucophage.” Also, establish relationships with pharmacists early – they’re incredibly valuable allies who can help coordinate transfers and catch dangerous interactions.
When New Medications Clash with Old Ones
Post-accident, you might suddenly find yourself on pain medications, muscle relaxants, anti-inflammatories, or sleep aids. These newcomers don’t always play nice with your existing medications. We’re talking about real interactions here – not just feeling a bit drowsier, but potentially dangerous combinations that could affect your heart, liver, or breathing.
The scary part? Sometimes these interactions don’t show up immediately. You might feel fine for days or weeks, then suddenly experience unexpected side effects. Meanwhile, you’re trying to document everything for insurance, and you can’t tell if symptoms are from the accident, the medications, or the stress of dealing with everything.
This is non-negotiable: Every single doctor needs to know about every single medication you’re taking. Not just the “important” ones – everything. Vitamins, over-the-counter pain relievers, that melatonin you take sometimes… all of it. And yes, this includes marijuana if you’re in a legal state and using it for pain management.
Keep that master list updated and bring it to every appointment. When doctors say “any medications?” don’t rely on your memory. Hand them the list.
The Gradual Medication Creep
Here’s something that sneaks up on people: medication creep. You start with one pain medication after the accident. Then maybe add something for sleep because the pain keeps you awake. Then perhaps an anti-anxiety medication because dealing with insurance is stressing you out…
Before you know it, you’re taking medications you never intended to take long-term. Each one made sense at the time, but now you’re looking at a handful of pills wondering how you got here.
The tricky part is that tapering off medications often needs to happen gradually and under medical supervision. You can’t just stop – but you also might not need everything forever.
Stay proactive about this. Every few months, have an honest conversation with your doctor about what you’re still taking and why. Some medications are meant to be temporary bridges while you heal. Others might be long-term necessities. Knowing the difference helps you plan for your recovery and your insurance documentation.
Setting Realistic Expectations for Your Claim Timeline
Let’s be honest here – dealing with medication coverage after an auto accident isn’t exactly a sprint. It’s more like… well, think of it as waiting for your doctor’s office to call you back, but multiply that by about ten and add some insurance companies into the mix.
Most people expect their medication claims to wrap up in a few weeks, maybe a month tops. But here’s the reality check you need: straightforward cases typically take 3-6 months to resolve, and that’s when everything goes smoothly. If there are complications – disputed liability, multiple parties involved, or questions about whether your medications are truly accident-related – you’re looking at 6-12 months, sometimes longer.
I know, I know. That’s not what you wanted to hear when you’re already dealing with pain and trying to get your life back on track. But understanding these timelines upfront can save you a lot of frustration down the road.
What “Normal” Actually Looks Like
During those first few weeks after filing your claim, you might feel like you’re shouting into the void. Phone calls that don’t get returned, paperwork that seems to disappear, adjusters who ask for the same information three times… Unfortunately, that’s pretty standard.
Here’s what typically happens in the early stages: The insurance company will assign an adjuster (this alone can take 1-2 weeks), they’ll start their investigation, and then – the waiting begins. They’re gathering medical records, reviewing police reports, maybe even hiring investigators if the accident circumstances are unclear.
Your medication claims are usually part of this bigger picture. The adjuster needs to understand your entire injury situation before they start approving ongoing treatment costs. It’s frustrating, but there’s a logic to it – they want to see if your prescriptions align with the injuries documented in your medical records.
Staying Organized While You Wait
This is where being your own best advocate really matters. Keep detailed records of every medication expense, even that $12 co-pay for your muscle relaxers. Take photos of receipts (trust me, they fade), maintain a simple spreadsheet with dates and amounts, and keep all your prescription bottles.
Actually, that reminds me – I’ve seen people get tripped up because they threw away old prescription bottles. Don’t do that. Those labels contain important information about dosages, prescribing doctors, and fill dates that might become crucial later.
Also, document how your medications are affecting your daily life. Are the pain meds making you too drowsy to work? Is the anti-inflammatory helping but causing stomach issues? These details might seem minor now, but they can strengthen your case for compensation later.
When Things Get Complicated
Sometimes your claim hits snags that extend the timeline significantly. Maybe the other driver’s insurance company disputes fault, or there’s a question about whether your current medications are related to pre-existing conditions versus accident injuries.
If you were already taking similar medications before the accident – say, for chronic pain or anxiety – expect extra scrutiny. Insurance companies will want to parse out what’s “new” versus what was already part of your medical routine. This isn’t necessarily them being difficult (though it can feel that way); they’re trying to figure out what they’re actually responsible for covering.
Your Next Steps Right Now
First things first – make sure you’re not paying out of pocket for accident-related medications if you can avoid it. Many people don’t realize they can often get their health insurance to cover prescriptions initially, then seek reimbursement from the auto insurance later. Check with your health insurer about this option.
Keep taking your prescribed medications as directed, even if the insurance situation is messy. Your health comes first, and gaps in treatment can actually hurt your claim later on.
Document everything, but don’t let record-keeping consume your life. Fifteen minutes a week updating your files is usually sufficient. Set a phone reminder if you need to.
And finally – stay in communication with your attorney if you have one, or with the insurance adjuster if you’re handling this yourself. A brief check-in every few weeks isn’t being pushy; it’s being appropriately persistent.
The medication piece of your accident claim might take longer than you’d like, but with realistic expectations and good organization, you’ll navigate this process successfully. Your focus should be on healing – the paperwork will sort itself out eventually.
Moving Forward With Confidence
Here’s the thing about dealing with medication coverage after an auto accident – it doesn’t have to feel like you’re navigating a maze blindfolded. Sure, the insurance world can be confusing (and honestly, sometimes downright frustrating), but you’re not meant to figure this out alone.
Your medications matter. Whether we’re talking about pain management, muscle relaxers, or specialized treatments your doctor prescribed… these aren’t luxuries. They’re essential tools in your recovery toolkit. And you deserve to have them covered properly without jumping through endless hoops or draining your savings account.
The process might feel overwhelming right now – I get it. One day you’re going about your normal routine, and suddenly you’re dealing with insurance adjusters, medical bills, and questions about coverage you never thought you’d need to ask. But remember this: every step you take to protect your medication coverage is an investment in your healing process.
Don’t let anyone rush you through decisions about your claim. Take the time you need to understand what’s covered, what documentation you’ll need, and how long that coverage might last. Keep those receipts, maintain detailed records, and don’t hesitate to ask questions – even the ones that feel obvious. Insurance representatives should be able to explain things in plain English, not insurance-speak that requires a decoder ring.
If you’re feeling stuck or confused about any part of this process, that’s completely normal. The intersection of healthcare, insurance, and legal claims isn’t exactly everyday knowledge. Some people find it helpful to work with professionals who understand these systems inside and out – whether that’s a personal injury attorney, a patient advocate, or even calling your doctor’s office for guidance on documentation.
And here’s something worth remembering: your health journey doesn’t pause while insurance companies sort things out. If you need your medications now (and of course you do), there are often interim solutions available. Don’t suffer in silence while waiting for claim approvals.
We’re Here When You Need Support
Look, managing weight loss goals while dealing with an accident injury adds another layer of complexity to everything. Your body is trying to heal, your routine has been disrupted, and now you’re juggling insurance claims on top of it all. That’s… a lot.
If you’re wondering how all of this affects your wellness plan, or if you need guidance on maintaining your health goals during recovery, we’d love to help. Sometimes having someone in your corner who understands both the medical side and the practical realities of insurance coverage can make all the difference.
You don’t have to have all the answers figured out before reaching out. Maybe you’re not even sure what questions to ask yet – and that’s perfectly okay. We’ve walked alongside many people through similar situations, and we know how to help you protect both your immediate medication needs and your long-term health goals.
Give us a call when you’re ready. No pressure, no complicated intake process – just real support from people who genuinely care about your wellbeing.